Introduction.
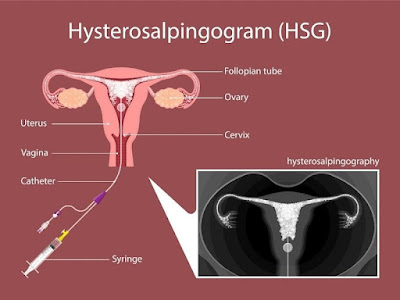
HSG is an X ray test which is done to see the outline of the shape of the uterus and to check if the fallopian tubes are blocked or open.
It is a minor procedure in which a special dye is injected that fills the uterus and then spills through the open fallopian tubes.
When Should this test be done
- As a part of workup for infertility.
- Usually recommended when a couple has been trying for more than a year with no success and when other basic tests have already been done.
- It is done after the periods ends but before the expected ovulation usually on cycle day 8 or 9.
Procedure
- The procedure takes around 15-20 minutes and is usually done in x ray department.
- The woman is made to lie on a bed that is positioned so that a x ray imager is above, that can take pictures during the procedure.
- The gynecologist will do an internal examination and then places a speculum in the vagina.
- The cervix is visualized then cleaned and then a cannula like devise is placed into the opening of the cervix.
- Then through this cannula a liquid dye that contains iodine is slowly injected to fill up the uterus.
- This dye can be seen on the Xray as a white image.
What Abnormalities can be detected on HSG
- Abnormalities like polyps or fibroids inside the uterine cavity can be seen.
- The shape of the uterus is outlined and any abnormal shape can be detected.
- The length of the fallopian tubes and if they are open by the spill of the liquid dye confirms the patency.
Is it Painful?